“Homelessness is like a black hole,” described Reginald Black, a long-time Street Sense vendor who is both trained to administer the city’s vulnerability assessment tool to determine who receives limited housing assistance, and who has been assessed himself.
Aware of the limitations of the coordinated entry system since it first began, Black is still patiently waiting for housing. He understood that the assessment tool was and is still in need of more resources and funding, coordination improvement and increased accountability.
In December 2015, the D.C. Interagency Council on Homelessness (ICH) acknowledged that most of the housing placements that occurred during the two-week, widely-publicized standoff and public shutdown of the “Camp Watergate” tent community happened outside of the coordinated entry system. While some were concerned that the most visible, rather than the most vulnerable, were receiving housing — others considered it a moot point, saying that unsheltered people should be given priority as well.
Currently, homeless encampments are still being removed underneath Deputy Mayor of Health and Human Services Hye Sook Chung, who took office in January. Neither Chung’s or Mayor Bowser’s office have replied to requests for comment beyond previously given statements of wishing to maintain public safety and health for all District residents while performing outreach to displaced persons.
Today, such placements no longer occur outside of the system, according to Emily Buzzell, director of outreach at Miriam’s Kitchen. Many people living in tent communities near Miriam’s, for instance, have not been matched with vouchers because they did not score high enough on the vulnerability index.
Buzzell pointed to how the collective accountability of the District’s system, while not perfect, has progressed and been successful. “[It] is a constantly evolving process. Honestly, it didn’t exist a few years ago, so we had to create a system out of nothing. It wasn’t going to be perfect the first time around and it’s still not perfect, so that’s why we have the ICH leadership team … constantly talking about what can we tweak to improve upon things.”
The need for a far more robust system and protocol for helping homeless individuals and families, either at the local or federal level, was reiterated by Scott McNeilly of the Washington Legal Clinic for the Homeless. “The question becomes,” McNeilly said, “can an individual sue to enforce federal guidelines?” The federal government provides regulations and standards that jurisdictions must meet in order to receive funding. However, localities are largely reliant on holding themselves accountable.
D.C.’s Mental Health Providers Are Struggling
While housing placements have sped up overall under the system — one particular group still remains in a tough spot: those refusing help who are not an immediate danger to themselves or others. Most often, that means people with mental illnesses.
Ward 7 Councilmember Vincent Gray began the April 28 Department of Behavioral Health budget oversight hearing with a statement criticizing the mayor’s lack of investment in mental health services.
“I’m deeply concerned about the three-year pattern of disinvestment in behavioral health services that we’re seeing from the mayor, culminating in this fiscal year 2018 budge,” Gray said. “There is a stark reduction in funding that is going out to our community service providers.”
Gray continued to spell out how the non-personnel services budget drops from $143.1 million in fiscal year 2015 to $123.8 million for 2018, a cut of about 13.5 percent. Examining the mayor’s proposed budget for DBH, funding has, indeed, stagnated over the last few years with little change despite the District’s growing need.
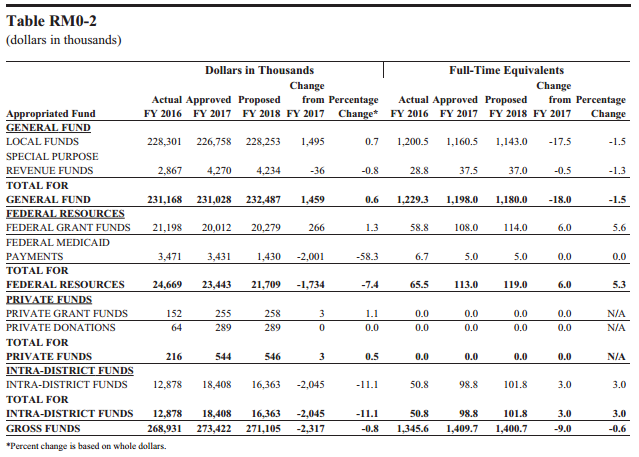
With this round of D.C. Council markup sessions for the budget ending on May 18, advocates and representatives of mental health service providers are calling for the mayor to substantially increase funding for mental health services.
“This should raise alarms about the behavioral health service provider system,” said Richard Bebout, former CEO of the now-closed Green Door Behavioral Health. Green Door was one of the District’s oldest mental health service providers until this past February when it closed down, mainly due to financial difficulties, according to Bebout. He also stated that there are many structural problems providers such as Green Door face just to make ends meet, especially with D.C.’s lack of safety net programs and full enforcement of mental health parity laws.
For example, the Green Door Clubhouse provided social, educational and employment programming but had to be shut down in 2010 primarily due to city budget cuts at the time. Bebout pointed to the nationwide problems and unintended consequences of the growth in Medicaid mental health spending which led many state governments to favor Medicaid funding for public mental health care and sparked a nationwide trend in underfunding non-Medicaid services.
Notably, Street Sense vendor and Green Door client Kanell Washington passed away in October 2016 from kidney failure. Washington had done “everything right,” according to his social worker, but the gaps in his care at Green Door — teams not following up, errors in paperwork, caseworkers not showing up more than six times — led to Washington ironically receiving a housing voucher (only from switching to Miriam’s Kitchen) the day after his death.
Over two hours of testimonies at the April 28 DBH budget oversight hearing included clients of Good Hope Institute wiping away tears while testifying that their opioid treatment will be cut off if they are unable to pay and numerous advocates in support of increasing youth mental health services and accountability over the DBH’s use of funds.
Dr. Tanya Royster, director of DBH, fielded questions at the hearing from the council and emphasized that DBH had reached out to providers multiple times to advise them to never summarily turn away people from treatment. Royster stated that some of the providers have been cooperative whereas others have not.
Hearing begins at 6:42.Video courtesy of the D.C. Council archive.
D.C. council also followed up on DBH’s investigation into Green Door’s closure. Royster said DBH’s new Chief Operating Officer, who started in March, is tasked with auditing Green Door’s records and drafting recommendations to guide future agency assessments of providers’ fiscal health. While there have been initial email exchanges between Bebout and the DBH, to date, the agency has yet to complete the investigation.
Councilmember Gray stated that it was his understanding that MBI Health Services, the company assuming control of Green Door’s former property, government contracts and operations, had made job offers to more than 90 percent of former Green Door employees and that most had accepted. Bebout explained to Street Sense, however, that while it was his hope that as many people as possible were able to transition to MBI in order to keep the same caseworkers and staff together with their clients — only about half of Green Door’s staff were offered jobs and many refused to accept MBI’s significantly decreased benefits and salaries.
“I wouldn’t be surprised if more organizations like Green Door closed down,” Bebout said, highlighting the continuing stagnation in funding for mental health services. Bebout himself has decided to pursue other opportunities rather than transition to MBI.
Clients’ Rights and The Rise of Community Mental Health Providers
Beginning in the 1950s, especially as the American public became aware of poor conditions in mental institutions, states shifted from central institutions to community-based care. In 1975, the O’Connor v. Donaldson Supreme Court ruling set the tone for many localities to adopt an “immediate danger” baseline — physical harm to oneself and others — for involuntary treatment.
Today, many psychiatrists and advocates such as those at the Treatment Advocacy Center, which is headquartered in Arlington, V.A., fear that America has deinstitutionalized far too quickly without building up enough local community resources.
Lisa Dailey, TAC’s legislative and policy counsel, wrote in an email to Street Sense that while TAC believes that “the laws in D.C. (together with legal interpretation) do allow for more robust use of inpatient and outpatient civil commitment, the practice has lagged behind what the law allows and has led to some situations where very sick people are allowed to languish without treatment.”
A Legislative or Humanitarian Touch?
Gunther Stern, executive director of Georgetown Ministry Center, sat quietly across the table, contemplating his retirement after decades of helping homeless people in Georgetown — after years of knowing that, under the District’s current mental health system, some people will never get off of the streets.
These are the people that cannot be helped through the coordinated entry system, according to Gunther. Not with assessments, not with housing placements and not with vouchers. These are the people of the District living with health problems and mental illnesses, the people now cynical and burned out of the system.
Ken Martin went through three separate vulnerability assessments and waited since 2003 for housing, due to a low vulnerability score despite being an elderly man with health problems that include multiple heart attacks and surgeries, spinal stenosis, peripheral neuropathy and torn meniscus. It is painful for Martin to just be on his feet and walking.
Martin only recently received a housing voucher through a dedicated person at the D.C. Office on Aging. “‘Mr. Martin,’ he recalled her saying, ‘you need this voucher. We don’t want you to die out there.’ She thought I was worthy, that I was deserving, that my children needed their father alive, and she wanted to do what she could do to help me.”
Sasha Williams dealt with depression and bipolar disorder alongside caring for her infant child as a single, homeless mother. With her baby in her arms, in the winter, Williams had been turned away from the Virginia Williams family resource center because the temperature was not below 32 degrees Fahrenheit exactly. Like with Martin, one dedicated person helped Williams get into a shelter on that winter night, connected her with another case manager in order to take the assessment again and followed up with Williams on the progress of her housing placement. Williams now has a federal voucher for a two-bedroom apartment and is looking to relocate soon.
Pete Earley forced his adult son, Kevin, into the hospital multiple times to receive treatment for his mental illness. After years of unraveling the nation’s mental health system to help his son, Earley, a 14-year veteran journalist, published his book “Crazy: A Father’s Search Through America’s Mental Health Madness” and regularly speaks out about how America’s prisons unofficially became the nation’s new psychiatric institutions and of how involuntarily committing his son ultimately led to saving Kevin’s life.
Bebout, Earley and Stern all stressed the significant difference early intervention has in a person with mental illness. By taking care of the person four to five years before they reach that “immediate danger” state is critical to prevent that person from deteriorating into a state too far gone, according to Bebout.
Stern criticized DBH’s policy of not intervening unless the person is in a dire state. “‘This person is ok because they’re not eating their feces, they’re not about to kill themselves, we can’t intervene’—and I think they could intervene … we need to do more.”
Stern discussed how people on the streets most likely have anosognosia, a lack of self-awareness about one’s own disability, such as a mental illness. They all advocate for the current emergency evaluation bar to be lowered so that people can receive treatment much sooner, whether voluntarily or not.
“But I’m not talking about locking up people forever, that’s inhumane,” Earley said in a phone interview, “I’m talking about caring about the person and taking them somewhere where you can provide them with good care until they’re stable.”
Earley spoke of his son who is now a peer support recovery specialist. Kevin is thankful that his father aggressively fought for his treatment, which included multiple hospitalizations, police tasering and arrests. They were worth it in order for Kevin to realize that he needed to become an active part of his own treatment.
“I don’t believe anyone is too far gone,” said Stephanie Lyons, a senior outreach specialist at Pathways to Housing D.C. Five years in, Lyons still sees herself continuing her daily work of constant outreach to clients.
Often it will take her years of frequent greetings, conversations and questions before the people she reaches out to finally open up and accept help. She described coming across many individuals with severe and persistent mental illnesses and negative experiences with the system. Building trust and rapport is difficult without constant, determined effort.
“The little successes can be the most rewarding and, you know,” Lyons said. “I’ve had clients say to me — it’s not necessarily ‘I appreciate you because you got me into housing, because you helped me get benefits,’ it’s more ‘I appreciate you because you didn’t give up on me, and that to me is what this work is all about.”
Lyons emphasized that this humanitarian element is essential to truly help people on the streets. But she also nodded in agreement when asked about the need for immediate medical attention to help people with extreme illnesses.
“But at some point, you got to get the person to want to change,” Earley said, “and that’s coming face to face with the real beast — the illness.”
Jeanine Santucci contributed reporting.